Frozen shoulder, also called adhesive capsulitis, is one of the most frequently seen shoulder problems. Unfortunately the frequency seems to be increasing. Those with frozen shoulder, usually have significant pain and restricted motion. Fortunately, the symptoms often resolve on their own. In many cases, treatment can frequently reduce the symptoms. However, in persistent cases, surgery is sometimes needed to improve or resolve the problem.
Frozen shoulder, also called adhesive capsulitis, is one of the most frequently seen shoulder problems. Unfortunately the frequency seems to be increasing. Those with frozen shoulder, usually have significant pain and restricted motion. Fortunately, the symptoms often resolve on their own. In many cases, treatment can frequently reduce the symptoms. However, in persistent cases, surgery is sometimes needed to improve or resolve the problem.
Frozen Shoulder: Anatomy
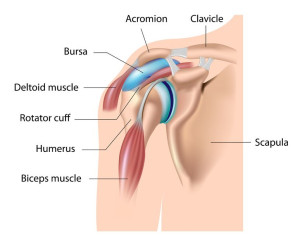
The shoulder is a ball and socket joint made up of two major bones, the upper humerus (ball) and the shoulder blade with the glenoid portion (socket). These bones are connected by the capsule and the capsules thickened portions, the ligaments.
A group of four deep tendons, the rotator cuff, are responsible for active shoulder motion. Lying on top of the rotator cuff and under an outcropping of the shoulder blade, the acromion, is the subacromial bursa. This bursa is a thin filmy sac that protects the rotator cuff during shoulder motion.
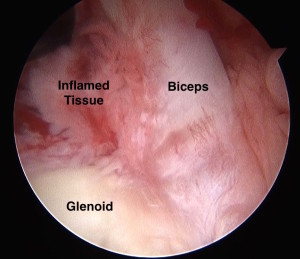
In frozen shoulder, the lining of the shoulder, the capsule, becomes inflamed and shortens. Consequently, there often is a significant reduction in shoulder motion as well as an increase in deep shoulder pain.
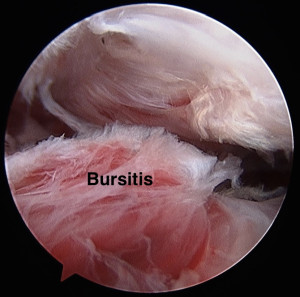
Additionally, due to the tightened tissues, the humerus tends to rise excessively with shoulder motion. This causes the subacromial bursa to get “squeezed”. The bursa then swells and becomes inflamed as a result. Consequently, even worsening pain often develops. The bursa extends down the arm some. So the bursitis often leads to pain on the side of the arm.
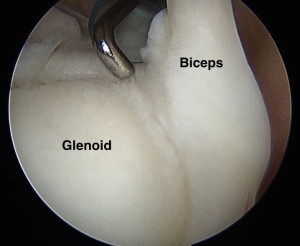
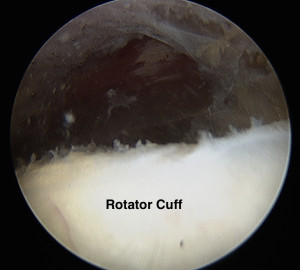
View the video below to see an arthroscopic view of the normal shoulder and a shoulder with frozen shoulder.
Frozen Shoulder: Risk factors
The exact cause of frozen shoulder is unknown. There are suspicions that it may be related to an issue with small blood vessels in the capsule (“vasculitis”). There is also some belief that there may be a dietary affect. What we do know is that there are certain groups that seem to have a predisposition to developing frozen shoulder. Among these are: Those with treatment-diabetes-info.com or thyroid disorders, middle-aged women, and those who’s shoulder motion has been restricted, such as those recovering from a stroke, women who have had surgery for breast cancer, men who have had cardiac bypass surgery or those who have had an injury to or surgery on their shoulder. With this said, a large number of those who develop frozen shoulder are not a member of any of these groups.
Fortunately, in many cases, frozen shoulder resolves on its own. Nonetheless, there are some treatments that can make you more comfortable while this occurs. However, unfortunately, patients, on occasion, get stuck and the symptoms don’t improve. For these cases, there is a surgical solution that can help.
I will discuss the symptoms of frozen shoulder and the treatment options, including surgery, in more detail in future posts. Until then, if your shoulder is stiff and you have noticed progressing pain, you may have adhesive capsulitis. So, it’s probably a good time to see a sports medicine shoulder specialist.