 Root tears are unique types of meniscal tears. In previous posts, we have discussed the various types of meniscal tears, mainly degenerative and traumatic. Additionally, we discussed a specific type of tear – the bucket handle tear. Now I’d like to discuss another kind – the root tear.
Root tears are unique types of meniscal tears. In previous posts, we have discussed the various types of meniscal tears, mainly degenerative and traumatic. Additionally, we discussed a specific type of tear – the bucket handle tear. Now I’d like to discuss another kind – the root tear.
What Are Root Tears?
The menisci are two soft cartilage c-shaped discs that exist in your knee between the end of your thigh bone (femur) and the top of your shin bone (tibia). They are connected from front to back in your knee. They are fixed peripherally and centrally to the lining (capsule) of your knee by soft tissue attachments. The front and back ends of the meniscus, are connected directly to the top of your tibia bone. These connections are called the roots. It is here where root tears occur.
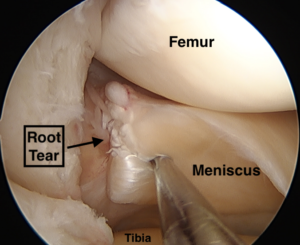
Root tears can be complete avulsions of the meniscus from the bone – the root pulls off the bone (see picture). They can also exist as partial or full tears through the tissue of the meniscus adjacent to the bone. Usually, root tears occur at the meniscal attachment in the back of your knee – the posterior root. More rarely they can occur at the root attachment in the front of your knee – the anterior root.
Who Gets Them?
Several groups of people get root tears more commonly than others. However, anyone can get a root tear. Like other meniscal tears, root tears can be degenerative – occurring slowly over time from age and “wear and tear.” They can also be traumatic – occurring acutely in relatively healthy tissue from a mishap. There are also variances of these two types that don’t fit perfectly into either group.
Degenerative root tears often occur in the presence of arthritis, usually in older people. Traumatic root tears are seen frequently in association with ACL tears but can result from any activity or injury that causes other traumatic meniscal injuries. Degenerative tears often occur at the posterior root of the meniscus. Root tears associated with ACL tears are more common in the lateral (outside) meniscus. A very common subgroup of patients that get root tears, almost always medial and posterior ones, are older obese women with early or advanced arthritis.
What Are The Symptoms Of Root Tears?
The classic symptoms associated with isolated root tears often include an acute “pop” in the back of the knee. Usually, this is followed by significant pain, swelling, reduced motion, and difficulty walking. Over several weeks, severe pain and swelling may improve. The pain in the back of the knee often persists, however. It is particularly bothersome with walking or twisting.
Why Are They So Bad?
Root tears virtually eliminate the protective function of the injured meniscus. Having a root tear is like not having any functioning meniscus on that side of your knee.
Why is this bad for your knee?
Your meniscus serves many functions. Among these are reducing the forces caused by the two main bones of your knee pressing against one another. The cartilage that protects the ends of these bones is sensitive to pressure and degenerates when it is excessive. Degeneration of cartilage is what we call arthritis. Arthritis can cause disabling pain and a slew of other symptoms that can adversely affect the quality of your life and ability to perform many of your activities.
Since the meniscus is no longer working to protect your cartilage when you have a root tear, the cartilage can deteriorate rapidly and lead to rapid and early arthritis. In fact, up to 30-50% of people who sustain a root tear require a knee replacement within five years. Not everyone will. But often they can, and that is why these injuries are so worrisome.
Not only can root tears cause arthritis, but arthritis can cause root tears. As the knee degenerates, everything in the knee degenerates, including the meniscus. As the knee goes through this deterioration, the space between the bones collapses. The collapse can then “squeeze’ the meniscus, lead to a tear of the root and “push” the meniscus out of the knee (extrusion). In this case, the root tear may not be a source of your symptoms but can be an ominous sign of a more significant developing problem – progressive arthritis.
How Are They Diagnosed?
For those of us who frequently treat meniscal tears, this diagnosis is often suspected simply from your description of your injury and symptoms. As mentioned above, usually there will be a “pop” in the back of your knee with persistent pain in that same location. On exam, there may be fluid in the knee (effusion), some initial stiffness and often very focal bone or joint tenderness on the side of the knee where the tear is.
X-rays are critical – not so much for the diagnosis, but to help eliminate other sources of pain, particularly evidence of preexisting arthritis. Also, once a tear is diagnosed, X-rays are essential in helping to direct the appropriate treatment.
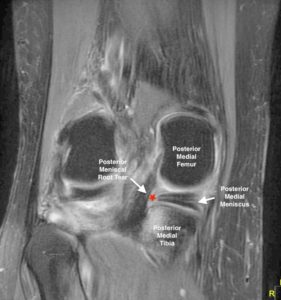
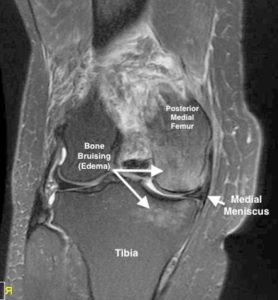
An MRI is diagnostic. It usually will show the tear clearly. It can also identify the extrusion of the meniscus if present. Furthermore, there may bone bruising (edema) in the adjacent bones from the acute trauma or increased stress on the bone due to the meniscus no longer functioning. Finally, MRIs can define the extent of preexisting arthritis. This information is critical in determining the proper treatment plan.
What Are The Treatment Options For Root Tears?
Work is still underway to determine how to treat these injuries in all cases. There are three options: Observe the tear, and only treat the symptoms, remove the torn piece (Meniscectomy), and repair the root back to the bony attachment.
Several factors determine the best treatment. There are the usual surgical ones: health, willingness for surgery, etc. There are also others specific to root tear treatment. The presence of knee arthritis, quality of the meniscal tissue, and the patient’s ability or desire to comply with a postop repair regimen (no or limited weight-bearing on the surgical leg x 4-6 weeks) are some of the more critical considerations.
Meniscal Repair
There are two reasons for surgery: 1) Reduce or eliminate pain, and 2) Prevent arthritis. Meniscal repairs in general and root tears specifically are performed to not only end the symptoms but also to prevent the development of osteoarthritis. We are unable to reverse or slow down the progression of arthritis once it exists. So, if you already have significant knee arthritis, there is no reason to repair your root tear. However, if there is mild arthritis or arthritis in a location distant from the injury, a repair may be considered. If no arthritis exists and you are able and willing to follow the postoperative restrictions and recovery timeline, a repair of the tear is often the preferred option.
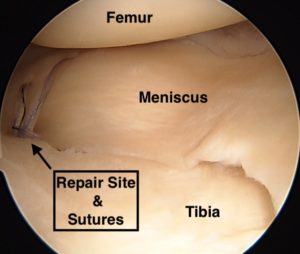
The video below shows an arthroscopic meniscal root repair.
Meniscectomy
What about trimming the torn piece?
Trimming the meniscus may provide some short-term relief of your pain and swelling. however because a root tear renders the meniscus nonfunctional, the long-term results differ from other types of meniscal tears treated this same way.
Whereas in other meniscal tears, removing small pieces of the meniscus is often a reliable treatment, that same approach in root tears has a worse long-term outcome. When removing a small portion of other types of meniscal tears, the function of the meniscus is often only partially reduced depending on how much of the meniscus is involved. Furthermore, many of these tears would not heal even if repaired.
With root tears, the situation is much different. Removing the piece may improve your pain, but since the meniscus is functionless without repair, the knee will often progressively deteriorate, sometimes rapidly. That’s not to say it never should be done, but like other surgeries, you should know what the surgery can accomplish and what to expect going forward. When treated in this fashion, many of these will have the same mid- to long-term outcome had no surgery been performed. As a result, often when a repair is not feasible or desirable, observation and symptomatic treatment, despite not preventing further knee deterioration, maybe the best option for you.
I was a professional table tennis player in china. I still actively playing. I am a 63-year-old man at 82 kg of weight. 2 years ago, I was injured in my left knee and it never fully recovered, I got lot of pain after games. 2 weeks ago, I was diagnosed via MRI with a root tear of the medial meniscus in the left knee, the meniscus is pushed out of the right place. my Dr. in China advice me to do the HTO. but I would like to ask if its possible to repair the root and reset my meniscus in the right place. I would to email you my MRI photo.
See reply on prior question.
I have my MRI photos in my handy computer.
I was a professional table tennis player in china. I still actively playing. I am a 63-year-old man at 82 kg of weight. 2 years ago, I was injured in my left knee and it never fully recovered, I got lot of pain after games. 2 weeks ago, I was diagnosed via MRI with a root tear of the medial meniscus in the left knee, the meniscus is pushed out of the right place.
my dr in china advice me to do the HTO. but I would like to ask if possible to repair the root and reset my meniscus in the right place. i would email you the MRI photo
It mostly depends if there is arthritis in the joint or not. If there is, repairing the meniscus will not help. That is what it sounds like by your doctors recommendation for an HTO. That is primarily done for arthritis. If you like to send the images, I’d be glad to take a look.
I have my MRI photos in my handy computer.
I was a professional table tennis player in china. I still actively playing. I am a 63-year-old man at 82 kg of weight. 2 years ago, I was injured in my left knee and it never fully recovered, I got lot of pain after games. 2 weeks ago, I was diagnosed via MRI with a root tear of the medial meniscus in the left knee, the meniscus is pushed out of the right place.
Hi Dr. Berg,
I ask for your help please. I need to find a surgeon to repair root tears of my medial meniscus. Besides this I have grade 2 runners knee on the medial side. I live in the Denver, CO metro area, but I can travel to your location as needed. Currently I am about 168 lbs, and a 5′-8″ woman, and I am on a diet to lose a lot of weight. I have always been an athletic person.
I have a current MRI report, and can I send this to you please/, and I had multiple falls while hiking/walking. Thanks for your help and this website!
Frab
I am sorry to hear about that. I am sure that there are a number of wonderful surgeons closer to you than me. I would suggest asking for an orthopaedic practice near you and asking the docs if they perform the procedure. I would caution you though. You alluded that you are trying to lose weight. We believe that one of the factors that cause these meniscus to fail and tear is excessive body weight. If repaired in this case, they may not heal or may retear. For that reason depending on a lot of factors, excessive body weight can be a relative contraindication to surgery.
Dr. Berg,
Sorry for another email. This is Fran Spicer from Denver Metro area. Please disregard my last email, and I believe the surgeon that got angry and said I definitely do not have a root tear is wrong. I researched root tears further, and I confirmed that I do have a root tear. I have had two MRI’s, and in 11-2019 MRI, said I have a root tear. 5-2020 MRI said that I had 5mm extrusion. I also noticed a case study with exact MRI results that I have and had a root tear.
I am sure I will need to go out of state for a surgeon for this repair at this point. I am loosing weight and was over 200 lbs when this happened, and now 166 lbs, and working on loosing much more weight. I will need to work from home, and will need a doctor’s help with a medical note. I currently live on the third floor, and will need to move out anyway.
Sorry for the emails, but I am not finding any surgeons that are knowledgeable.
Thanks for your help and it is appreciated! Fran
Dr. Berg,
What tx is there if one has a root tear and arthritis in the knee area, not sure how bad, but let’s worst case it?
Thank you.
If you have very bad arthritis with a root tear, the treatment is directed to the arthritis and not the root tear. The issue is a much bigger problem than just the meniscal tear. Our data shows us that treating just the root tear does not effect the course of deterioration of the knee and progression of the arthritis. Often there is no improvement if treating the meniscal tear, even in the short-term. I discussed the treatments for arthritis here: https://www.jeffreybergmd.com/arthritis-diagnosis-and-treatment/
Hello!
I haven’t found info on internet how medial meniscus root retear could happen. I was in surgery where they fixed my acl with hamstring graft and medial meniscus root tear. I was sent out without brace and toe touch weight bearing. After like few days of surgery when i did some of the PT exercises i wanted to try how my hamstring is working and i could move my leg just a small amount and it was super hard as expected but now i read from internet that you shouldn’t try to activate hamstring after meniscus root repair. Is it possible i made some harm to repaired root?
Root tears can occur along with ACL tears. I do not usually restrict hamstring activities after root repairs. I do restrict weightbearing and knee bending while weightbearing. Although I can’t assess your root repair specifically, typically, the activity you describe would not be worry me.