 Do you have arthritis? Has someone told you that you might be a candidate for subchondroplasty? What is subchondroplasty? What does it treat? How does it work? Let’s take a look…
Do you have arthritis? Has someone told you that you might be a candidate for subchondroplasty? What is subchondroplasty? What does it treat? How does it work? Let’s take a look…
In a prior post, I described what osteoarthritis is. In short, osteoarthritis is a degeneration of your joint. It affects the bone, soft tissues and primarily the cartilage lining the bones. The most common cause is age-related deterioration. It can also result from an acquired or congenital joint deformity, following trauma, surgery or joint infection. There are some treatments for symptomatic osteoarthritis. Among the available treatments is a slew of nonoperative options and surgery. Surgical options include joint replacement, arthroscopy alone or arthroscopy with subchondroplasty.
Why add Subchondroplasty?
Like all medical issues, arthritis can come in different patterns. Some folks respond to some treatments, and some respond better to other treatments. Consequently, patients with arthritis sometimes don’t get adequate relief from any nonsurgical therapies and their only options for alleviating their symptoms may be surgery. Often these patients may be contemplating a joint replacement. A subset of these patients may respond to a subchondroplasty, and therefore they would be able to avoid joint replacement…at least in the short-term.
Who responds to Subchondroplasty?
As mentioned earlier, arthritis is the wear or absence of cartilage, that white, glistening, smooth coating covering the ends of your bones at your joints. This cartilage, when healthy, protects the bone ends. Unlike the underlying bone that is full of nerve fibers, cartilage has no nerve fibers, and so when present and healthy, the bone is not only shielded from excessive forces but pain as well.
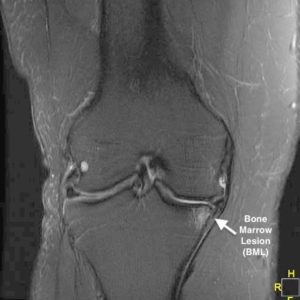
When worn or absent, cartilage can’t protect the bone as much, or even at all. In that case, changes in the bone from repetitive or excessive forces often can cause pain. On occasion, these forces can cause “bone bruises.” These are small fractures in the bone marrow. Sometimes these fractures are acute injuries, and sometimes they are more chronic, stress fractures. MRI imaging studies reveal these injuries as bone marrow lesions (BMLs). These BMLs can be very painful. Often they will resolve with time. But sometimes they don’t…
If your BML persists on an MRI and symptomatic beyond three months, a subchondroplasty may be right for you. By symptomatic, what we are talking about is pain and tenderness precisely at the location of the bone injury. Often with arthritis, patients will have diffuse pain – that is they will have pain all over the knee. These more diffuse symptoms would not respond to subchondroplasty.
Most commonly, this problem occurs in the knee. So subchondroplasty is mostly used in the knee joint. However, BMLs can occur in other joints as well. Likewise, subchondroplasty can also be used in the shoulder, hip, and ankle too. Finally, patients can sometimes develop similar symptomatic BMLs without arthritis. In those cases, a subchondroplsty may also be helpful.
What is Subchondroplasty?
A subchondroplasty is an outpatient, minimally invasive procedure that aims to stabilize the bone marrow lesion and therefore reduce (and hopefully eliminate) any pain generating from that area. During the surgery, your surgeon will insert a thin tube through a tiny skin incision into the area of the bone injury. An x-ray-like machine is used to assist in positioning the tube. A semi-liquid substance containing calcium is then injected through the cannula and into the lesion. The substance hardens into a chalk-like substance within minutes. The hardened material has strength characteristics of healthy bone marrow, and it also has a structure that promotes bone ingrowth and ultimate replacement by your bone.
Your surgeon will almost always perform arthroscopy along with the subchondroplasty. The arthroscopy allows us to identify and address any potentially treatable issues inside the joint. It also allows us to remove any of the injected substance that might inadvertently get into the joint through the uncovered bone.
What happens after the Subchondroplasty?
As mentioned this is typically an outpatient procedure. So you can go home the same day. Immediately after surgery, you are permitted to put all your weight on your surgical leg. You may feel weak or unsteady doing so, and so crutches or a cane may be needed for several days – occasionally for a couple of weeks – depending on your progress. A brace is not typically required. Usually, there is only a small soft dressing. The dressing is generally removed after a couple of days. Likewise, removal of the few needed stitches usually occurs in about a week.
Most patients will begin physical therapy within a couple of days and continue this for several weeks. In the appropriately selected patients, improvement often starts in 2-6 weeks. Full recovery may take 3-4 months, however. Overall for most patients, it is a relatively safe procedure with risks similar to isolated knee arthroscopy.
Who shouldn’t have Subchondroplasty?
Any medical issues that would prohibit a simple arthroscopy would also preclude proceeding with a subchondroplasty. Furthermore, this surgery is inadvisable for anyone with active infection in the joint of concern.
Subchondroplasty is ineffective when there is advanced arthritis in the joint. Similarly, those patients with diffuse arthritic pain without corresponding bone lesions in the areas of pain or patients without any BMLs on their MRI would be unlikely to benefit from subchondroplasty.
What are the results of Subchondroplasty?
There have not yet been much research on this procedure. But there is some. One recent small, short-term study showed that the most significant improvement in pain and function occurred within two weeks of surgery. These improvements mostly continued for six months after surgery. Another more extensive paper has demonstrated similar results. In this study, the positive outcomes continued for two years at which time the study period ended. Finally, this procedure has been shown to reduce the need for knee replacement in those who had been considering a knee replacement before their subchondroplasty.
Higher level studies with a comparison to patients treated without subchondroplasty are getting underway (here and here). Hopefully, these will give us more information about subchondroplasty’s efficacy. I’ll let you know when the data is available.
What’s the take-home message about Subchondroplasty?:
I need a hip replacement on my left hip. I am 69 years old and have a full titanium pin in my left femur. Is Subchondroplasty at all possible with the pin in place to relieve my hip pain? The hip is Arthritic.
Mr. Melina, obviously it is difficult to give specific answers as I don’t know all the details of your particular case. Although subchondroplasty can be an option in hip arthritis, It is used to only address any symptoms that maybe there from painful bone marrow lesions. this is usually the exception, not the rule. Typically there is diffuse arthritis and the symptoms are due to limitations in range of motion and diffuse arthritis. In those cases, subchondroplasty would not help much, if at all. I suggest discussing with your surgeon about your particular case.
I have a stress fracture in my right hip with a lot of pain. I’ve been told I need a total hip replacement. I’ve been doing research on SCP and wondering if this procedure would be an option.
Hard to say without knowing all the details and reviewing images. I suggest you ask your surgeon or get another opinion and get a thorough evaluation and discuss all your options and ask all your questions. Best of luck.
Are there Physicians offering this treatment in SW Ohio and is it typically
covered by insurance.
I am sure that there are physicians in SW Ohio who perform the surgery. However i do not know any to recommend. It is typically covered by insurance if performed for stress fractures and bone marrow lesions. These are essentially micro fractures and therefore billing for the necessary arthroscopy and fracture fixation is usually accepted.
I had it done 2 weeks ago for severe bone edema and a stress fracture in my heel! So far it’s been a disaster and I am wondering if my severe osteoporosis coupled with my vitamin D deficiency has something to do with it?
I’m sorry to hear that. Those issues you mentioned are often responsible for stress fractures. Without knowing the details of your case, I cannot even guess when you might be having such problems. I suggest discussing this with your surgeon or seeking a second opinion. I wish you good luck.
Hello sir, my left hip is going weak . I can’t walk like other and pain is high.I have face so many doctors of india all have suggested me to hip change. Is this therapy is useful for me. If yes then it will be miracle for me. I want to know
Neelash, As I tried to note in the post. This procedure is only helpful for a small subset of patients with arthritis. Unfortunately, I do not treat patients with hip arthritis. My suggestion would be to discuss this with your doctors and ask them their thoughts. I wish you the best of luck.
Hello Dr., my mother (71 YO) was diagnosed with arthritis, she has almost perfect mobility but the joint is damaged. She also has pain frequently. Could this procedure be an option? Thank you
Gisela, It is possible. Subchondroplasty can treat a small subset of people with hip arthritis. Usually they have an acute onset of increased symptoms. However most people of your mother’s age who have hip arthritis not adequately treated by nonoperative means, require a hip replacement to treat their problem.In order to know if a person is a candidate or not, an MRI of the hip and an evaluation by an Orthopaedic surgeon who treats hip arthritis would be required. Best of luck.
Who in Orange County,Ca diagnoses whether a Pt is a candidate for sunchondroplasty and if they are diagnosing the Pt as a good candidate are they also the Dr that most likely will perform the procedure
I’m sorry, I have no way of knowing who performs this procedure anywhere. I am not aware of any list. It is relatively common. I would suggest calling an orthopaedists office who speciallizes in knee surgery and asking. Best of luck.
Doc I have had one hip replacement due to what I refer to as being a human german shepherd. Basically I was told my hip did not form completely and thus I have worn the cartilage out on the top of the hip joints. I am guessing this might not be an option for my other hip as it has the same condition but thought worth asking as I am always looking for the latest and greatest.
Sounds like you had Dysplasia. Yes German Shepard’s get it too :). Hard to say from here without an exam or imaging what would be best for you specifically but generally people with that issue are better served with a hip replacement.
Hi Dr Berg,
Do you know anyone Ortho doc in the Tampa, FL/St Petersburg/Saraota, FL area that performs this procedure on the hip? I’ve been treating my hip pain (osteo-arthritis) with stem cells over the last 2 years with good results looking for an alternative to total hip replacement. I’m 58 and would like to wait to get a hip replacement. Any help would be greatly appreciated. I already have my ct scan on my hip.
I’m sorry. Unfortunately, I do not. Best of luck in your search.